A method for imaging and characterizing the esophageal wall using a tethered capsule has been developed by researchers from Harvard Medical School and Strasbourg University. The technology, which uses optical coherence tomography (OCT), may provide a simple and convenient method for diagnosing upper gastrointestinal tract diseases such as Barrett's esophagus (Biomedical Optics Express, February 2016, Vol. 7:2, pp. 409-419).
The diagnosis and subsequent treatment of many diseases of the upper gastrointestinal tract often call for endoscopic examination. Unfortunately, this is typically expensive, uncomfortable, requires patient sedation, and only provides limited information on surface tissues. Subsequent biopsies can provide additional information, but only from limited sample sites. This can be especially problematic when attempting to diagnose diseases with patchy presentations, such as Barrett's esophagus -- in which esophageal tissues change to resemble those that line the intestine.
One alternative is to use OCT, an imaging technique that uses backscattered, near-infrared light -- in a manner analogous to ultrasound -- to create micron-resolution images. In their work, Harvard Medical School's Dr. Guillermo Tearney, PhD, and colleagues have developed an OCT capsule for imaging the esophagus.
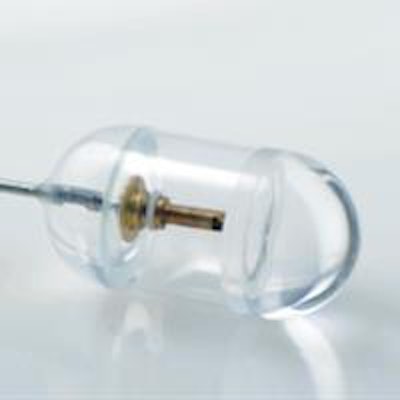
 The swallowable tethered capsule endomicroscopy device comprises a small capsule attached to the end of a thin flexible tether. The tether encloses an optical fiber that delivers light from the OCT system to the capsule. The fiber is terminated with micro optics that redirect and focus the light immediately outside of the capsule's housing. All images courtesy of Dr. Guillermo Tearney.
The swallowable tethered capsule endomicroscopy device comprises a small capsule attached to the end of a thin flexible tether. The tether encloses an optical fiber that delivers light from the OCT system to the capsule. The fiber is terminated with micro optics that redirect and focus the light immediately outside of the capsule's housing. All images courtesy of Dr. Guillermo Tearney.As the capsule is swallowed, or retracted by its tether, it creates 360° cross-sections up and down the esophagus. From the data generated, it is possible to distinguish between regular and abnormal tissues. Being only 11 x 24.5 mm in size, the capsule can be easily swallowed. Compared with endoscopy, this makes the procedure more comfortable for the patient -- who need not be sedated -- and simpler, as it can be performed in a nonspecialized setting without a physician.
Data analysis
The capsule device comes with some technical challenges, however, the most problematic being the time-consuming nature of manually characterizing the data collected. To address this, Tearney and his team have developed a computer algorithm capable of mapping the imaged tissues and identifying the presence of Barrett's esophagus. In a clinical trial, the algorithm's tissue characterization produced a 94% match with those conducted manually by an expert.
Furthermore, the automated system can provide feedback to the capsule operator about the level of tissue contact between the capsule and the esophageal wall. The highest quality images are produced with full contact, which is typically ensured by peristalsis, but can be lost if the esophagus expands. As the capsule can be easily re-engaged by giving the patient a sip of water, however, this feedback capacity will allow sections to be re-imaged if needed and ensure a complete dataset is acquired.
"This study demonstrates that tethered capsule OCT endomicroscopy images of abnormal esophagus can be discriminated from normal esophagus using an automated computer software algorithm," Tearney said. "[This] is one important step that moves us closer to using tethered capsule endomicroscopy as a widespread screening test for Barrett's esophagus."
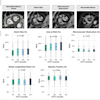
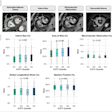
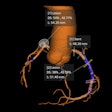
 Images from the OCT capsule reveal differences between Barrett's esophagus and squamous (normal) esophagus.
Images from the OCT capsule reveal differences between Barrett's esophagus and squamous (normal) esophagus."We have seen many endoscopic advances in the detection and treatment of precancerous cells in the esophagus in the recent years. Despite the success of these tools, we are still faced with the problem that most of the patients who present with esophageal cancer are diagnosed at advanced stages when the prognosis is poor," commented Dr. Vani Konda, a gastroenterologist at University of Chicago Medicine who was not involved in this study. "Tethered capsule endomicroscopy has the potential to be an efficient, nonendoscopic screening tool to identify those who may benefit from an upper endoscopy and to fill a gap in our current screening paradigm for Barrett's esophagus."
Having demonstrated its potential, Tearney and colleagues are now moving to further develop their screening technology, with an eye to decreasing processing times and conducting comparisons between their algorithm's output and histopathology as the gold standard. They are also investigating whether this technique might also be used for the diagnosis of other gastrointestinal tract cancers and conditions such as allergic esophagitis and coeliac disease. According to the researchers, the technology might find wide clinical application within a few years.
© IOP Publishing Limited. Republished with permission from medicalphysicsweb, a community website covering fundamental research and emerging technologies in medical imaging and radiation therapy.