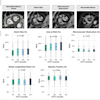
Patients at risk of developing hepatocellular carcinoma (HCC) should be enrolled in an ultrasound surveillance program, noted Irish researchers in an award-winning e-poster presented at the 2013 European Society of Gastrointestinal and Abdominal Radiology (ESGAR) annual meeting in Barcelona.
If a focal liver lesion is discovered on surveillance ultrasound, subsequent investigations must be decided based on lesion size, according to lead author Dr. Lisa Lavelle, a specialist radiology registrar from St. Vincent's University Hospital in Dublin, who received a cum laude award for her exhibit at last month's congress.
In her practical guide to HCC, she also urges radiologists and other staff to remember that ancillary features of HCC include restricted diffusion and lack of uptake of liver-specific contrast media; Barcelona Clinic Liver Cancer (BCLC) is the staging system of choice linking stage with treatment; stage 0 and A are potentially curative treatments, stage B and C improve life expectancy and quality of life; and the modified Response Evaluation Criteria in Solid Tumors (mRECIST) guideline can be used to assess tumor response to locoregional therapy, including assessment of tumor necrosis.
HCC is the sixth most common cancer worldwide, and cirrhosis is the strongest predisposing risk factor, according to the authors. The causes of cirrhosis include chronic viral hepatitis, alcohol, hemochromatosis, alpha-1-antitrypsin and nonalcoholic steatohepatitis. The risk of HCC is highest in viral hepatitis, and one-third of cirrhotic patients develop HCC during their lifetime.
"HCC is a unique tumor commonly diagnosed on imaging features alone due to its characteristic enhancement pattern and arterial hyperenhancement with delayed washout," they stated. "High-risk groups include cirrhotic patients Child-Pugh A and B, cirrhotic patients Child-Pugh C awaiting transplant, noncirrhotic hepatitis B virus carriers with active hepatitis or positive family history for HCC and noncirrhotic patients with chronic hepatitis C and advanced liver fibrosis."
Most nodules less than 1 cm detected within cirrhotic livers are not HCC, and if a focal lesion is identified within a cirrhotic liver, follow-up imaging is determined by the lesion size, they added.
Noninvasive HCC diagnosis should be based on the identification of the characteristic enhancement pattern in a cirrhotic liver on either CT or dynamic contrast-enhanced MRI, particularly arterial hyperenhancement with washout in the portal venous or delayed phase. If this enhancement pattern is present on a single four-phase examination, it fulfills diagnostic criteria for HCC in lesions greater than 2 cm, noted Lavelle and her colleagues. Ancillary features suggestive of HCC include restricted diffusion and lack of liver specific contrast uptake; these features are not included within the diagnostic guidelines at present, but may be helpful for small hypovascular HCC.
"Caution is required when giving definitive opinions on nodules measuring 1-2 cm unless using high quality technology in a specialist center. For the general radiologist, EASL-EORTC (the European Association for the Study of the Liver and European Organization for Research and Treatment of Cancer clinical practice guidelines) advocate consideration for performing a second four-phase test for lesions measuring 1-2 cm," they explained.
"Contrast-enhanced ultrasound is not recommended as an alternate diagnostic modality. The microbubbles remain in the intravascular space in contrast to iodinated contrast and gadolinium, which are cleared from the intravascular space into the extracellular space resulting in diagnostic overlap with intrahepatic cholangiocarcinoma exhibiting a similar enhancement pattern to HCC," they added.
A biopsy is recommended for nodules in noncirrhotic livers, as well as if imaging findings are inconclusive or atypical in the setting of cirrhosis. Stromal invasion is the differentiating feature between high-grade dysplastic nodules and early HCC. There is also a 2.7% risk of tumor seeding postbiopsy, they concluded.
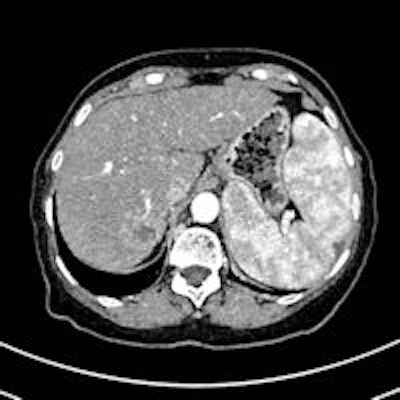
Editor's Note: The image on our home page is of a patient with several HCC nodules. CT scan after transarterial chemoembolization (TACE) shows the necrotic lesion. Courtesy of Dr. Christoph Zech, University Hospital Basel, Switzerland; previously published in ECR Today 2013 congress newspaper.