The incorporation of contrast-enhanced ultrasound (CEUS) adds a critical dimension to the evaluation of scrotal diseases, prize-winning researchers from a top U.K. university hospital have reported.
“Its unique ability to conclusively demonstrate the absence of vascularity is essential for diagnosing global or segmental infarctions and identifying hematomas or abscesses, allowing more informed clinical decision-making and improving both diagnosis and management outcomes,” noted Dr. Faiz Jabbar, clinical radiology registrar at King's College Hospital NHS Foundation Trust in London, and colleagues.
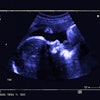
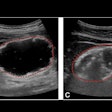
 Scrotal trauma. After a 45-year-old man underwent sperm retrieval from the left testis for management of infertility, he presented with continuing pain following the procedure. The B-mode ultrasound (a) demonstrated a serpiginous low reflective area in the mid aspect of the testis (arrow). On the color Doppler examination (b), some shunting of blood (arrow) was visible to the lateral aspect of the low reflective area. On the contrast-enhanced ultrasound examination (c), the shunt was again noted (arrow) and the area of hematoma formation was visible (star). All figures courtesy of Dr. Faiz Jabbar, Dr. Dean Huang, and Prof. Paul Sidhu and presented at ECR 2025.
Scrotal trauma. After a 45-year-old man underwent sperm retrieval from the left testis for management of infertility, he presented with continuing pain following the procedure. The B-mode ultrasound (a) demonstrated a serpiginous low reflective area in the mid aspect of the testis (arrow). On the color Doppler examination (b), some shunting of blood (arrow) was visible to the lateral aspect of the low reflective area. On the contrast-enhanced ultrasound examination (c), the shunt was again noted (arrow) and the area of hematoma formation was visible (star). All figures courtesy of Dr. Faiz Jabbar, Dr. Dean Huang, and Prof. Paul Sidhu and presented at ECR 2025.
CEUS is of great value in definitively identifying the absence of vascularity in scrotal imaging, and it aids clinical decision-making across various scrotal pathologies and informs management and follow-up, they explained in an e-poster exhibit that received a certificate of merit at ECR 2025.
“A key strength of CEUS lies in its ability to conclusively differentiate vascularized from nonvascularized components of scrotal contents,” they stated. “The technique’s capability to depict vascularity at the capillary level, combined with its use of a purely intravascular contrast agent that does not leak into the extravascular space, improves the assessment of lesion vascularity.”
CEUS is particularly useful for detailing the presence or absence of vascularity in focal testicular tumors, ascertaining viable tissue in trauma, detailing the extent of a segmental infarction, and ascertaining the configuration and site of an abscess, the researchers pointed out.
Technique and practical tips
After identifying a scrotal abnormality using initial greyscale and color Doppler ultrasound, CEUS is employed. The procedure involves a bolus injection of an ultrasound contrast agent, administered via a 22-gauge cannula inserted into the antecubital vein, they stated.
The most widely used product for the assessment of scrotal disease is Lumason/SonoVue (Bracco), a sulfur hexafluoride microbubble contrast agent. The examination requires a higher dose of the microbubble contrast (4.8 mls of Lumason/SonoVue) because the physics of the harmonic response of the microbubble is governed by the acoustic properties in the insonating ultrasound field, with the smaller microbubbles required to interact with the higher frequency beam found at a smaller concentration.
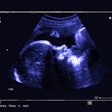
 Epididymal abscess. A 56-year-old man with underlying diabetes mellitus presented with a left-sided scrotal mass and pain. On the B-mode ultrasound (a), a 20 x 22 mm mixed reflective mass was present in the epididymis (arrow). The color Doppler ultrasound (b) showed a lack of vascularity within the abnormality (arrow), with the contrast-enhanced ultrasound (c) showing absence of enhancement and vascularity centrally (star) and surrounding hyperemia (arrows). An epididymal abscess was present with reduced symptoms in an immuno-compromised diabetes mellitus patient.
Epididymal abscess. A 56-year-old man with underlying diabetes mellitus presented with a left-sided scrotal mass and pain. On the B-mode ultrasound (a), a 20 x 22 mm mixed reflective mass was present in the epididymis (arrow). The color Doppler ultrasound (b) showed a lack of vascularity within the abnormality (arrow), with the contrast-enhanced ultrasound (c) showing absence of enhancement and vascularity centrally (star) and surrounding hyperemia (arrows). An epididymal abscess was present with reduced symptoms in an immuno-compromised diabetes mellitus patient.
Harmonic imaging is used with a low mechanical index (MI), typically set at or below 0.10, and a frame rate of 10-20 frames per second during the enhancement phase. “The initial CEUS examination, occurring within the first two minutes after injection, is critical for capturing meaningful diagnostic information,” they said.
When performing CEUS, specific technical considerations are essential for optimal imaging. A split-screen approach, displaying B-mode and CEUS images side by side, allowing low-MI B-mode images to localize the area of interest. The focus should be set deep into the target area, and the gain should be adjusted before injecting contrast. Precontrast images should appear nearly black, according to Jabbar and colleagues.
The dynamic range can be set wide to capture fine differences in enhancement or narrowed to make blood vessels appear brighter. Mechanical index should be carefully managed, as excessively high MI can disrupt microbubbles in the near field, while too low MI results in poor visualization of the far field.
“Video clips should always be recorded for re-evaluation,” they emphasized . “CEUS examinations are safe but require precautions due to the rare risk of anaphylactic reactions, necessitating prompt access to resuscitation equipment.”
Scrotal cysts and lesions
Epidermoid cysts -- composed of keratinizing, stratified squamous epithelium with a well-defined fibrous wall -- represent a subset of complex cysts. “These lesions are rare, constituting approximately 1% of testicular masses, and are often asymptomatic, palpable, and detected during routine physical examinations. Their ultrasound appearance varies depending on the maturation, compactness, and quantity of keratin present,” the researchers explained.
Characteristic patterns include an “onion ring” appearance of alternating hyperechogenicity and hypoechogenicity, an echogenic mass with dense acoustic shadowing due to calcification, or a target-like mass with a central echogenic area surrounded by a hypoechoic periphery, they noted. “CEUS consistently demonstrates the avascular nature of these lesions. In cases where an epidermoid cyst is strongly suspected based on imaging, testis-sparing enucleation may be an appropriate management option.”
 Epidermoid cyst. A 19-year-old man with a history of nonspecific pain was found on ultrasound (a) to have an incidental lesion in the left testis (arrow) with features suggesting an epidermoid cyst. There was no color Doppler (b) signal in the lesion (arrow). On the contrast-enhanced ultrasound (c) exam, there was no vascularity within the lesion (arrow).
Epidermoid cyst. A 19-year-old man with a history of nonspecific pain was found on ultrasound (a) to have an incidental lesion in the left testis (arrow) with features suggesting an epidermoid cyst. There was no color Doppler (b) signal in the lesion (arrow). On the contrast-enhanced ultrasound (c) exam, there was no vascularity within the lesion (arrow).
CEUS is highly reliable for assessing scrotal lesions, but there are rare exceptions where its ability to demonstrate the lack of enhancement requires careful interpretation, the authors noted. “Extensively necrotic lesions may exhibit little to no enhancement due to the absence of vascularity within large areas of tissue death,” they said.
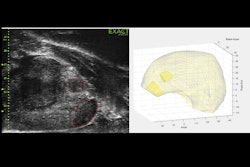
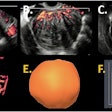
 Infarcted tumor -- pure seminoma. A 41-year-old man with a 48 x 30 mm right testicular mass, which was an avascular infarcted tumor with multiple small vascular satellite lesions. The lesions were of low reflectivity (arrows) and did not demonstrate increased flow on microvascular imaging (a). On contrast-enhanced ultrasound (b), the large lesion was avascular (star) and the smaller inferior lesion (arrow) had abnormal enhancement, with increased early arterial enhancement and subsequent rapid washout in keeping with a germ cell tumor. On histology, this was found to be a pure seminoma.
Infarcted tumor -- pure seminoma. A 41-year-old man with a 48 x 30 mm right testicular mass, which was an avascular infarcted tumor with multiple small vascular satellite lesions. The lesions were of low reflectivity (arrows) and did not demonstrate increased flow on microvascular imaging (a). On contrast-enhanced ultrasound (b), the large lesion was avascular (star) and the smaller inferior lesion (arrow) had abnormal enhancement, with increased early arterial enhancement and subsequent rapid washout in keeping with a germ cell tumor. On histology, this was found to be a pure seminoma.
You can read the full e-poster here. The co-authors were Dr. Dean Huang, Dr. Gibran Timothy Yusuf, Dr. Maria Sellars, and Prof. Paul S. Sidhu.