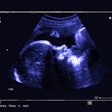
Results from a quality improvement (QI) initiative at the Mater Hospital in Dublin aimed at providing a snapshot of a workday in the ultrasound procedural room were presented as an e-poster at ECR 2025.
The study, performed by Dr. Jonathan Hunter and colleagues in the radiology department, was intended to highlight areas in need of improvement and suggest changes.
“[QI] initiatives are essential to enhancing patient care, optimizing workflow, and reducing operational inefficiencies,” they noted. “There is, however, no standard practice on how to run and optimize an ultrasound procedural room, and a lack of guidance can result in unnecessary delays to patient care.”
Both inpatient and outpatient ultrasound procedures at the Mater Hospital are performed within one room. On average, the authors wrote, the team aims to perform five procedures in the morning and three procedures in the afternoon.
Doctors both in and outside of the radiology department were asked to complete surveys. A range of satisfaction scores was provided for questions about the procedural room, including staff perceptions of patient care delays to overall satisfaction values of the service.
Prospective data for the study were collected over one month in July/August 2024; the focus of the data analysis was on average times calculated between key checkpoints in a patient's pathway from entering the department to leaving the procedural room.
For outpatients, the checkpoints included arrival at the hospital, entering the procedure room, completing the procedure, and leaving the procedure room. For inpatients, the first checkpoint was when the patient was called from the ward rather than his or her arrival at the hospital.
In addition, the team analyzed the average for how long the procedural room was empty between cases -- i.e., “deadtime.”
Following these analyses, “quick fixes” intended to improve efficiency were implemented, and data were reevaluated to determine if there were any improvements following the changes.
The findings showed specific breaks in the workflow that resulted in lost time, as well as gaps in communication with doctors. The most common issues identified included inefficiency in preparing a patient prior to their procedure, “deadtime” between procedures, and difficulty with communication between doctors and procedure room staff. The communication gap was underscored in the survey responses.
Although 90% of doctors found the ultrasound procedure room to be satisfactory overall, 75% expressed that the room was responsible for some delays in patient care; 20% said they experienced a significant delay.
“Following survey analysis, specialty teams found the procedural room satisfactory in providing timely intervention, however, commonly found communicating the urgency of procedures with radiology trainees to be their main frustration,” the authors noted.
Around 75% of doctors said that they had difficulty discussing “new urgent cases” with procedure room staff (usually as staff were preoccupied with the scheduled cases of the day) said that they were able to have their questions answered satisfactorily and their cases triaged appropriately once their queries were addressed.
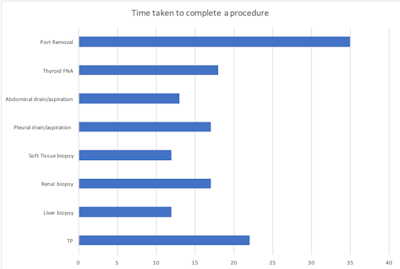 Breakdown of average procedural times. Figures courtesy of Dr. Jonathan Hunter et al and presented at ECR 2025.
Breakdown of average procedural times. Figures courtesy of Dr. Jonathan Hunter et al and presented at ECR 2025.
While procedure times were deemed satisfactory, the average time from the checkpoint of the patient being called to the procedural room to the completion of the procedure was 85 minutes. The wait time for patients prior to entering the procedure room was responsible for the long average timespan.
For outpatients, the average wait time to enter the procedure room after arriving was 49 minutes. Attending and preparing the patient for the procedure and waiting for the procedure room to be available accounted for most of the wait time.
For inpatients, the average waiting time for a patient to enter the procedure room was 64 minutes. Sending for the patient, awaiting porter availability, and “variable delays” in patients leaving the ward accounted for the majority of long wait times. Additionally, once the patient had arrived at the radiology department, there was an average wait of 19 minutes for the procedure room to be available.
Deadtime -- the periods when the ultrasound room was not in use -- consistently occurred most at the start of the day and to the cases before and after the 45-minute lunch break period; these periods averaged approximately 44 minutes. The overall downtime between cases (taking the lunch break into account) was 36 minutes.
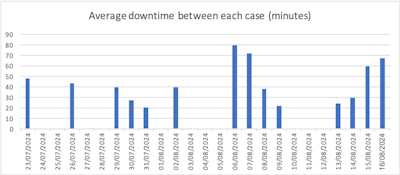 Downtime averages over several points within the month.
Downtime averages over several points within the month.
Furthermore, the authors noted, this inefficient use of time was in part due to another break in the workflow: “The mid-day deadtime was attributed to the morning staff predicting delays in patients arriving to the room, and thus not calling for an additional patient in case the procedure ran into the afternoon shift, thus extending the gap between both.”
Based on the findings, the “quick fix” solutions implemented for reducing delays included schedules created the day before to aid in efficient daily planning and reduce time spent preparing the patients for procedures, exploring separating inpatient and outpatient procedures to make workflow more efficient, creating requisition forms and online triage lists for staff, and better “communication pathways.”
These interventions resulted in better performance and optimistic data on improvement, the authors noted. More complex, long-term suggestions were proposed (including two dedicated rooms for inpatients and outpatients); however, the implementation of these solutions faces limitations such as staffing and funding.
“This snapshot into a month's work within the ultrasound procedural department highlights the need for basic guidelines on procedural management to reduce the potential inefficiencies caused by unregulated room structuring,” the QI team concluded, noting that the project also underscores the value such initiatives can have in creating structures and improving efficiency.
You can read the full ECR 2025 e-poster here. The co-authors of this study were Sine Gilchriest, Jane Burns, Sadhbh Doherty, Oliver O'Brien, Molly Godson Treacy, and Brian Gibney.