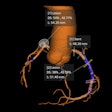
Having recurrent prostate cancer patients undergo gallium-68 (Ga-68) prostate-specific membrane antigen (PSMA) PET/CT can help direct clinicians to effectual curative treatment options that also are cost effective, according to a study by German researchers published in the October issue of the Journal of Nuclear Medicine.
The research group compared the outcomes for Ga-68 PSMA PET against carbon-11 (C-11) choline PET and contrast-enhanced CT for tumor, node, and metastasis (TNM) staging and recommended the first modality also become the standard strategy for assessing prostate cancer recurrence after surgery with or without radiotherapy.
"The main findings include the cost efficacy of Ga-68 PSMA PET by calculating the additional costs of wrong intended treatment occurring in approximately two of three patients after conventional CT staging," wrote lead author Dr. Johannes Schwenck and colleagues from Eberhard Karls University in Tubingen (JNM, October 2019, Vol. 60:10, pp. 1359-1365). "In addition, we were able to demonstrate that Ga-68 PSMA PET gave a high chance of curative treatment for patients without previous radiotherapy and new curative options in patients after previous radiotherapy, who usually would otherwise receive palliative androgen deprivation therapy."
The recurrence of prostate cancer is quite common, even among patients who have undergone surgery, radical proctectomy, or salvage radiotherapy. Better diagnostic accuracy through PET "could potentially circumvent this therapeutic gap," the authors wrote. "Therefore, we evaluated consecutive Ga-68 PSMA PET/CT, C-11 choline PET/CT, and standard CT imaging in the same patient with regard to TNM-stage migration."
For this study, they retrospectively analyzed 83 patients (median age, 69.3 years; range, 51-86 years) from December 2013 to December 2014 who underwent PET/CT scans with both Ga-68 PSMA and C-11 choline tracers. Subjects with prostate cancer recurrence had a median prostate-specific antigen (PSA) level of 1.9 ng/mL (range, 0.2-33.4 ng/mL) after radical prostatectomy. The median time difference between PET examinations and radical prostatectomy was 3.7 years (range, 0.2-21.2 years).
Both the Ga-68 PSMA and C-11 choline PET scans led to concordant results in 60 patients (72%). However, agreement with TNM staging between Ga-68 PSMA PET and diagnostic CT was only evident in 30 patients (36%). C-11 choline fared about the same, with concordance in only 33 cases (40%) with CT.
Curative treatment options were available in approximately half the patients who previously had undergone radiotherapy and in more than 90% of patients with no such treatment. Ga-68 PSMA PET correctly identified 57 patients who would benefit from curative treatment and 26 patients (31%) who were better off with palliative care. C-11 choline PET correctly identified curative treatment for 41 patients (72%), while CT offered an accurate assessment in only 19 cases (33%).
"In general, wrong treatment was usually associated with initiation of another (hopefully correct) therapy," the authors wrote. "Here, we assume that the more precise diagnostic procedure using Ga-68 PSMA leads to a better (i.e., correct) treatment."
To estimate the additional costs of a wrong treatment, Schwenck and colleagues based their calculations on Germany's reimbursement standards and adding the additional costs of wrong intended treatment occurring in approximately two of three patients after conventional CT staging. For example, a standard C-11 choline tracer would add 108,510 euros per 83 patients.
"Regarding costs avoided by use of the correct Ga-68 PSMA PET/CT-directed treatment, a Ga-68 PSMA PET/CT study would be cost-effective if the additional costs, compared with a C-11 choline PET/CT study, do not exceed 1,307 euros per examination," the authors wrote. "CT-standard staging would result in additional costs of 319,035 euros per 83 patients."