French experts have urged all clinical staff to keep aware that meningoencephalitis is a possible complication in patients with ZIKV infection (Zika virus), according to a research letter published in the New England Journal of Medicine. Radiology plays a pivotal role in the diagnosis of this complication, which if left undetected is likely to result in a patient's deterioration and even death, they noted.
The letter, posted on 9 March, described the case of an 81-year old man who was admitted to the intensive care unit at Henri Mondor Hospital (AP-HP Henri Mondor), Créteil, in France 10 days after returning from a four-week cruise through New Caledonia, Vanuatu, the Solomon Islands, and New Zealand, during which he was reported to be in perfect health. The man had a fever of 102.4° F (39.1° C) and was comatose; other symptoms included hemiplegia of the left side and paresis of the right upper limb.
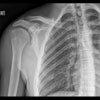
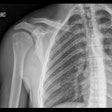
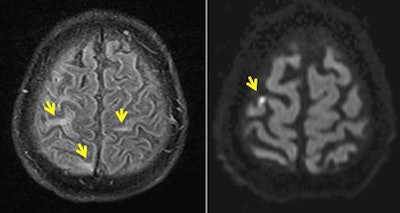 Left: FLAIR image shows multiple cortical hyperintensities in patient with Zika virus. Right: DWI reveals small infarct with restricted diffusion in same patient. Images courtesy of Dr. Pierre Brugières.
Left: FLAIR image shows multiple cortical hyperintensities in patient with Zika virus. Right: DWI reveals small infarct with restricted diffusion in same patient. Images courtesy of Dr. Pierre Brugières.An MRI scan of the brain suggested meningoencephalitis, with "asymmetric white-matter hyperintensities on fluid-attenuated inversion recovery (FLAIR) imaging, multiple punctuated hyperintensities on diffusion-weighted sequences that were evocative of ischemic foci, and a slight hyperintensity of the right Rolandic fissure that was evocative of meningitis," noted the authors. CT also showed an irregular narrowing of the right callosomarginal artery.
Further tests suggested meningitis, but tests of the patient's blood and cerebrospinal fluid (CSF) were not revealing. Ultimately, the Zika virus was grown in a culture from the patient's CSF on a cell line. This was the first case of Zika-associated meningoencephalitis at AP-HP Créteil.
The patient's condition continued to improve during his hospitalization, and he was discharged from the intensive care unit on day 17. His cognitive function was fully recovered by day 38.
MRI is always the first-line modality when dealing with suspected meningoencephalitis associated with infectious disease, explained Dr. Pierre Brugières, a senior neuroradiologist at AP-HP Henri Mondor who performed the patient's MRI with FLAIR and diffusion sequences.
"The main message is that in patients with Zika, radiologists should look for encephalitic lesions with MRI if central neurological deficits or consciousness disorder are observed. Morphological, diffusion-weighted imaging (DWI), and time-of-flight (TOF) sequences are key to diagnosis of meningoencephalitis which, if left undetected, would probably result in a worsening of impaired consciousness and death," Brugières told AuntMinnieEurope.com in an interview. "MRI allows us to check for brain infection by depicting parenchymal and subarachnoid space anomalies using FLAIR sequences. Furthermore, diffusion imaging may show subcortical ischemic stroke evocative of associated microvascular pathologies."
 Detection and characterization of encephalitic lesions with MRI can prove life-saving, Dr. Pierre Brugières said.
Detection and characterization of encephalitic lesions with MRI can prove life-saving, Dr. Pierre Brugières said.While parenchymal, subarachnoid, and vascular abnormalities on MRI are suggestive of meningoencephalitis, they are not specific to Zika, he continued. Meningoencephalitis may be observed in other infections such as tuberculosis, pyogenic meningitis, and cryptococcosis -- or in inflammatory diseases such as neuro-behçet disease. Lumbar puncture is necessary for differentiating infections and choosing the appropriate treatment path.
"We didn't know that the patient had Zika; it was the lumbar puncture that confirmed this. Indeed, while there is no specific treatment for Zika, an emergency-adapted antibiotic treatment is essential in the case of tuberculous or pyogenic meningitis," Brugières said.
He added that he had no idea of whether or not incidence of Zika, and Zika-related complications, would rise in France but as significant numbers of French citizens continue to travel to and from endemic regions, there was a risk that more cases like this could be seen in the future.
The clinician should consider encephalitis in a patient with the appropriate symptoms such as fever and loss of consciousness, he said, adding that while MRI could provide arguments for meningoencephalitis, the specific research for Zika should be performed if the patient has visited any geographical zone where the risk of Zika contraction is high.
"There is no specific treatment for Zika. Early recognition of meningoencephalitis allows appropriate supportive care and optimizes the overall treatment. MRI and CT were essential in this case, as in most meningoencephalitis cases, helping to precisely characterize the lesions, which in turn may influence the clinical reasoning and etiological hypothesis," stated Dr. Guillaume Carteaux, senior intensivist at AP-HP Henri Mondor, and lead author of the letter.
Zika virus infections have been known in Africa and Asia since the 1940s, but the virus' geographic range has expanded drastically since 2007 spreading across countries and territories, mainly in the Americas and the western Pacific, but also in Africa and Southeast Asia. The bite of Aedes aegypti mosquitoes is the chief means of transmission. Since 2013, contraction of Zika infection by pregnant women has been associated with an increase in fetal development abnormalities, including microcephaly, as seen in French Polynesia, and more recently in Brazil.