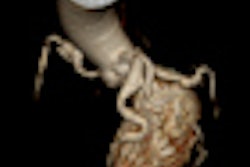
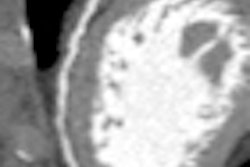
Incidentally detected findings at routine chest CT -- especially coronary and aortic calcifications -- are a strong predictor of future cardiovascular events, researchers from the Netherlands reported in European Radiology. Their study of more then 10,000 patients found a significantly higher rate of cardiovascular events in patients with the findings detected on ungated chest CT scans.
The findings suggest reporting and prevention of calcifications, and other findings, via a simple visual scoring system could potentially be used to alert patients to the presence of calcifications, and through preventive care, help prevent serious problems down the road.
Routine chest CT "provides numerous exemplary cases of unrequested information: vascular calcifications, pulmonary emphysema, pulmonary nodules, or skeletal osteoporosis," noted Drs. Peter Jacobs, Martijn Gondrie, Mathias Prokop, and colleagues from University Medical Center Utrecht , Elkerliek Medical Center Helmond, and Radboud University Nijmegen Medical Center in Nijmegen, the Netherlands (European Radiology, May 21, 2011).
Vascular calcifications are common in the normal populations and are frequently detected when reading diagnostic CT scans in clinical care patients. However, no follow-up studies have been performed to examine their prognostic value for cardiac events, the group wrote.
The study examined whether subclinical coronary and/or aortic calcifications detected at routine diagnostic chest CT are associated with future cardiovascular disease (CVD) events. A total of 10,410 subjects older than 40 were scanned at eight different hospitals. None had evidence of poor prognosis, cancer, or cardiovascular disease, conditions for which more than 20,000 patients had been excluded.
The CT scans were acquired between 2002 and 2005 using two-, four-, eight-, 16-, 40-, or 64-dector-row systems from various manufacturers. To be included in the study the scanned field-of-view had to include the heart and the full length of the thoracic aorta. Slice thickness varied depending on the indication, for example suspected pulmonary embolism 3 mm to 5 mm for standard chest CT, the authors noted.
The study employed a case-cohort study design with random sampling of a representative subcohort of about 10% of patients (n = 1,285) from the baseline 10,410 patients at the beginning of the study. The design "provides an efficient way to avoid scoring CT characteristics for all 10,410 subjects of the baseline cohort, but instead only in incident cases and a representative baseline sample," Jacobs and colleagues wrote.
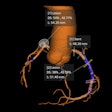
Images were examined in the axial plane by three experienced readers, who scored them visually for coronary and aortic calcifications. Each of the four main coronary arteries were scored separately (scale 0-3), then added into a single score for the coronary artery tree (0-12). The aorta was scored as to calcification in the ascending (0-3), descending (0-3), and supra-aortic arteries branching from the aortic arch (0-2) and added into a single score for the thoracic aorta (0-12).
They followed patients for both fatal and nonfatal cardiovascular events during a mean 17.8 months, with events defined by ICD-9 codes. End points were defined by National Death and hospital discharge registries. Statistical analysis used Cox proportional-hazard models to compute hazard ratios to predict cardiovascular disease events.
Stronger association for coronary versus aortic plaque
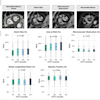
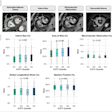
Coronary artery calcium (CAC) and aortic calcium (TAC) were both significantly and independently predictive of cardiovascular events, Jacob et al reported. The results show "a gradual increase in annualized event rate for any ... event with increasing CAC and TAC score categories," they wrote.
"Severe coronary (CAC) or aortic (TAC) calcification -- based on visual grading of calcified plaques -- increased the risk of any CVD event almost threefold and fourfold, respectively, after a mean follow-up of close to one and a half years," Jacob et al wrote. "CAC was found to be a stronger predictor of coronary events, whereas TAC was more strongly associated with noncardiac events."
The prevalence of coronary artery calcium was 67% for people in the subcohort compared with 88% among subjects who had cardiovascular events; 90% for those with coronary events, and 85% for patients who suffered noncardiac events (p < 0.001 for all three groups).
For thoracic aortic calcium the prevalence was 61% in the subcohort, 82% in subjects who had cardiovascular events, 80% for those with coronary events, and 86% for those who suffered noncardiac events (p < 0.001 for all three groups).
The results also showed a statistically significant increase in hazard ratio in the case of even mild calcification (TAC and CAC scores of 1-2). Compared with no calcification, the risk of any cardiovascular events rose by a factor of 2.7 for thoracic artery calcium (95% confidence interval [CI], 2.0-3.7) and 3.7 for coronary artery calcium.
Subjects with coronary and noncardiac events were older than people in the subcohort, but only subjects with coronary events were more often male.
The risk of coronary events increased fivefold among subjects with severe CAC (score ≥ 6) compared with those with no coronary calcium, while severe TAC (score ≥ 5) boosted the risk by a factor of 2.4.
Annualized event rates
|
||||||||||||||||||||
| From a total of 515 cardiovascular events during a mean 17.8-month follow-up period. | ||||||||||||||||||||
Aortic calcium was more strongly associated with noncardiac events than with cardiac events. The risk of noncardiac events (including stroke, aortic aneurysm, or dissection) increased by a factor of 3.3 for subjects with severe aortic calcium compared with patients with none, whereas those with severe CAC showed an increase in risk by a factor of 2.3. No statistically significant interaction was found between section thickness and TAC (p = 0.46) or CAC (p = 0.89), and the use of intravenous contrast and TAC (p = 0.40) or CAC (p = 0.81) in relation to the risk of CVD events.
As for aortic calcifications, the only association to reach statistical significance was in the ascending aorta. Moderate calcification of the ascending aorta increased the risk of stroke by a factor 3.0 compared with no calcification, whereas moderate calcification of the descending aorta or supra-aortic branches increased the risk by factors of 1.8 and 1.4, respectively, the authors wrote.
Although major advances in risk factors have been achieved, and international guidelines developed for the primary prevention of disease, "substantial groups of people at intermediate or high risk of CVD events according to existing guidelines are currently not recognized and treated as such," the group wrote. This gap has prompted a search for new strategies to detect patients who would benefit most from intensive primary prevention efforts, which is a clinically important objective. The present study is an attempt at defining such a new strategy.
Unrequested coronary and aortic calcifications detected on routine chest CT using a simple visual scoring system can predict future cardiovascular events, Jacobs et al concluded. Applied to routine practice, the method can be used to identify patients who could benefit from preventive efforts.