Treatment planning and evaluation in head and neck oncology represents a major challenge for the radiologist. But new techniques and protocols are helping to overcome obstacles, and promise much in treatment prediction and early follow-up, delegates discovered at Friday's European Congress of Radiology (ECR) Special Focus Session.
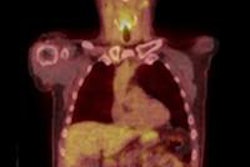
Insensitivity to treatment, induced fibrosis or inflammation, and aspecific metabolic effects of chemotherapy may complicate the choice of treatment and methods to assess its efficacy, but the continued growth in biomarkers and surrogate markers is causing excitement. The use of 18F-misonidazole for marking tumor hypoxia is gaining ground, as is PET/CT with F-FLT. FLT signal changes precede changes to tumor volume, a potential early marker for treatment response monitoring in oropharyngeal tumors. However, because of FLT take-up in reactive lymph nodes, issues remain over its incapacity to distinguish them from those which are metastatic.
 Dr. Vincent Vandecaveye from Leuven, Belgium.
Dr. Vincent Vandecaveye from Leuven, Belgium.
"New PET tracers should be handled with care," said Dr. Vincent Vandecaveye, from the department of radiology at Leuven University Hospitals in Belgium. "CT has very high negative predictive value for excluding residual disease. If you have small lymph nodes after radiotherapy, there is only a small chance that this will be nodal recurrence. We shouldn't forget the basics in this whole story. The question is not what to use, but when to use it."
Head and neck cancer is the sixth most common cancer, according to session moderator Dr. Alexandra Borges, from the Portugal Institute of Oncology in Lisbon, Portugal. More than 90% of these cases are squamous cell carcinoma (SCC). For unresectable advanced disease, the five-year survival rate is less than 10%.
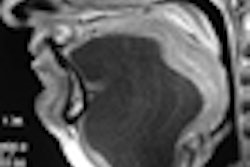
The importance of knowing expected findings postradiotherapy, and being able to distinguish unexpected findings from recurrence or residual tumor, could be facilitated through using a score of 1 to 3, noted Dr. Frank Pameijer, from the University Medical Centre Utrecht in the Netherlands. Expected findings post-treatment, such as edema, could be scored as least worrisome, or 1. The second score, 2, could be applied to focal masses smaller than 1 cm and asymmetry and necessary follow-up for up to two years, while the third category of findings (masses more than 1 cm or less than 50% in tumor reduction post-treatment) require immediate further investigation, either through biopsy or metabolic imaging.
 Dr. Alexandra Borges from Lisbon, Portugal.
Dr. Alexandra Borges from Lisbon, Portugal.
Pameijer urged post-treatment patience when following up for recurrence or residual tumor with PET/CT. Rather than imaging at one month after treatment, when negative predictive value was too low at 14% to 28% to yield valid results, radiologists should wait because negative predictive value increased to almost 100% after three to four months. Positive predictive value at that stage also increased to between 71% and 81%, making it accurate in eight out of 10 cases in real terms, allowing 80% of patients to avoid unnecessary therapy.
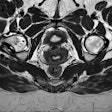
In comparison, diffusion-weighted imaging MRI can be performed after six weeks with a high negative and positive predictive value, but this relatively new technique means that few institutions have the experience necessary to use it for follow-up. Although instinctively doctors want to know post-treatment outcome, overall improved survival rates due to speedier detection of recurrence are yet to be proved.
 Dr. Frank Pameijer from Utrecht, the Netherlands.
Dr. Frank Pameijer from Utrecht, the Netherlands.
"We have to find out if it is beneficial to the patient to detect recurrence or persistent cancer after six weeks rather than after three months. Intuitively DW-MRI will see recurrence earlier, but it will take a lot of effort for centers to introduce it into routine practice," he said.
New imaging paradigms such as structural imaging to specify locoregional extent, functional and molecular imaging as surrogate markers of tumor biology could help tailor treatment, and provide early prediction of tumor response and dynamic-treatment tailoring, as well as prognostic information.
The aim is now to determine the best performing modalities for tumor staging, detection of occult and unknown primaries, predicting tumor response to conventional and new biologic therapies, and post-treatment follow-up.
Oncologic imaging is a top priority, European Society of Radiology (ESR) President Dr. Maximilian Reiser told attendees at the opening ceremony on Thursday evening. Plans are advanced for the formation of the European Society of Oncologic Imaging, which will be part of the ESR.
Originally published in ECR Today March 5, 2011.
Copyright © 2011 European Society of Radiology