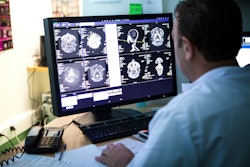
Repeated mistakes in how scans are read and acted on have led to delays in diagnosis and treatment, unnecessary surgeries, and avoidable deaths in the U.K. National Health Service (NHS), the Parliamentary and Health Service Ombudsman (PHSO) has reported.
In a press release issued on 20 March, the PHSO, which serves as the NHS’s watchdog, detailed examples of 45 cases involving such errors that the Ombudsman has upheld or partially upheld since publishing a 2021 reports on imaging failings in the NHS (see auntminnieeurope.com/clinical-news/article/15655758/uk-watchdog-calls-for-urgent-improvements-in-radiology-services).
The most common issues the PHSO identified were doctors failing to identify an abnormality, scans being delayed or not being carried out at all, and results not being properly followed up.
Examples of the consequences of the errors described by the PHSO included a 10-month delay in cancer diagnosis that significantly reduced the patient’s survival chances, an avoidable death caused by pelvic sepsis not being identified, and a missed ankle fracture resulting in an avoidable operation.
In one case, failure to report a small bowel lesion and subsequent repeated failures to diagnose a patient’s cancer led to delayed treatment and prolonged pain for the patient, who took his own life, citing the pain as the reason. The PHSO concluded that the errors made in the patient’s care probably contributed to the man’s decision to end his life.
The PHSO has highlighted these cases as a call for more learning to prevent the same mistakes being made, emphasizing that the responsibilities for these issues exist on a systemic level.
“Each of the cases we have investigated and upheld represents a real person whose life has been impacted by failings in care. They are also all instances where the organizations involved failed to identify that anything had gone wrong,” said Rebecca Hilsenrath, the lawyer who heads up the PHSO.
“When things go wrong, there must be learning at both an organizational and wider systemic level. In our 2021 report, we recommended a system-wide program of improvements for more effective and timely management of x-rays and scans. While we have seen some progress in this area, unfortunately, we are still seeing instances where people’s care is sub-optimal, often with devastating consequences,” he noted.
Reaction to PHSO report
For radiologists, the report may serve to not only highlight the need for learning from these errors but also the need to identify gaps in communication with others outside the field.
“This is a very distressing report, and not just because of the stories of individual patients who may have been harmed either by misdiagnosis or by failures in communication,” said Dr. Giles Maskell, consultant radiologist at Royal Cornwall Hospitals NHS Trust, Truro, U.K., and a regular columnist on AuntMinnieEurope.com.
“It appears to illustrate the gulf in understanding which now exists between radiologists and others of the nature of radiology as an interpretive process and the consequent inevitability of some level of error in our work," he told AuntMinnieEurope.com. "As a profession, we have developed a reasonably sophisticated understanding of these issues over recent years, but we have not yet managed to communicate this to nonradiologists and particularly to patients and the public at large. I believe this is a key task for our professional bodies.”
The Ombudsman highlights "some devastating failures in the NHS, and we must collectively learn from these experiences to drive meaningful change," said Dr. Kath Halliday, president of the Royal College of Radiologists (RCR), adding that the RCR is committed to supporting learning with guidance and educational resources and through the Radiology Events and Learning (REAL) initiative, which includes a platform where clinicians can submit anonymous cases that others can learn from, as well as an annual meeting where clinicians come together to reflect on and learn from mistakes.
"However, we must also recognise that these findings reflect a system that is overburdened and under-resourced," she continued. "We face a 30% shortfall of clinical radiologists, projected to rise to 40% by 2028. As the Ombudsman points out, inadequate digital infrastructure is a patient safety issue. We urge the government to act on these findings and invest in the capacity and infrastructure necessary to support NHS staff to give every patient the care they deserve.”
Read the PHSO’s statement and case summaries here.