In Germany alone, between 12 and 15 million people suffer from long-term or recurring pain, of whom around 4 to 5 million are severely impaired. Pain management is also an issue for radiology and was a central theme on the opening day of the 105th German Congress of Radiology, RöKo 2024, which takes place in Wiesbaden from 8 to 10 May.
This Q&A interview on the topic is with Prof. Philipp Paprottka, head of interventional radiology at the Rechts der Isar Clinic, Technical University of Munich, and president of the German Society for Interventional Radiology and Minimally Invasive Therapy (DeGIR).
Q: Why is the topic of pain management so important?
A: That's easy to answer: Pain affects many people and has a very negative impact on their quality of life. The suffering of those affected is great. That's why it's important to offer some hope to patients, e.g., those with chronic degenerative diseases as well as tumor-related diseases, ideally to eliminate or at least alleviate the pain and achieve a higher quality of life.
Q: At RöKo 2024, you're giving a lecture on "Aspects of radiological pain treatment." Which aspects are important?
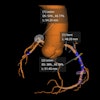
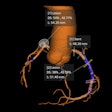
A: My lecture is about the variety of interventional radiological pain therapies. Most of us think of periradicular therapy and facet joint injections, but I would also like to introduce other, more specific therapies. Bone metastases, for example, are treated with a combination of radiofrequency ablation, vertebroplasty, injections, and radiation therapy, which leads to freedom from pain. In patients with pancreatic cancer in the palliative setting and with severe pain, the nerve fibers can be switched off using interventional methods to keep people pain-free in the last few months. We can now offer many therapies. Of course, it is also important to listen to the patients, talk to them, and discuss the procedure and more. It's not just about the technical stuff.
Q: Can pain management be improved through the use of AI?
A: Yes. By using AI, diagnostics can be made faster, better, and more effective. In interventional procedures, for example, we see progress through the further development of large-scale equipment, but also through the improvement of navigation, fusion systems, and methods used for controlling the interventions. An example here is CT angiography.
Q: What are the potential advantages and risks of using image-guided techniques to treat pain?
A: The main advantage is precision. For most pain therapies, we use CT to guide interventions. Of course, it would be desirable if this could be done using MRI because the soft tissue contrast is better, but MRI is less available and also significantly more expensive. Thanks to today's fusion options, the information from MRI can also be used for CT interventions.
The complications depend on the type of procedure. You have to clarify this individually for each patient, weigh up the benefits and risks, and then plan each procedure carefully. With pain therapies, the benefit for the patient in terms of quality of life is usually high and the risk is low. Most of the time there is only a small amount of bleeding in the access route.
Q: How effective are image-guided pain treatments? What new techniques are being developed?
A: Some of the therapies we offer can also be carried out without image guidance. There are very experienced colleagues who can do that. Personally, I am convinced that the therapy results are better if you can position the needle tip with millimeter precision under 3D visibility and monitor the distribution of the therapeutic agent in real-time. In my opinion, this has a positive effect on the outcome.
What is particularly noteworthy in this area is the further development of large devices and navigation software systems. Both lead to the expansion and improvement of procedures and fewer complications. There are also new procedures, for example, joint immobilization. This means that if patients have pain in their joints, it can be treated with the help of particles. With this method, those affected, who have often already exhausted the entire spectrum of conservative and surgical treatments for pain, can still be pain-free or procedures can be delayed.
Q: How do you ensure continuing education and training?
A: We take a two-pronged approach: We must train and further train young people so they can operate the complex systems in the future. At the same time, we also must give them basic skills so they can carry out interventions safely in locations that may not have the very best equipment.
Editor's note: This is an edited version of a translation of an article published in German online by the DRG. To read the original version, go to the DRG website.