The mammography landscape continues to evolve as new technologies enter the field. This is reflected in the European Commission (EC) breast cancer screening guidelines, which are continuously reviewed and updated to take into account the growing body of evidence that is being delivered to support these technologies.
The most recent update for breast cancer screening was issued by the EC in May 2023. This supported the use of digital breast tomosynthesis (DBT) in breast cancer screening programs, which is helping to positively shape screening practices across the region, marking a significant step forward. The updates have also set the stage for innovation and the integration of advanced screening tools as more facilities look to adopt DBT.
 Dr. Eva Pallwein-Prettner.
Dr. Eva Pallwein-Prettner.
By formally recognizing the advantages of DBT and acknowledging the extensive research highlighting its benefits for all women, not just those with dense breast tissue, the EC has helped propel its adoption, including in Austria, where it was approved for use in January 2023.
At our facility, we have embraced DBT as part of our standard practice. We have observed that the shift to DBT has yielded remarkable results, with enhanced spatial resolution and increased detection of microcalcifications, architectural distortions, and small lesions, particularly in dense breasts.
Data from clinical trials support this. DBT has been shown to detect up to 65% more invasive cancers than a 2D mammogram alone.1 Additionally, the Tomosynthesis plus Synthesized Mammography (TOSYMA) study found that DBT plus synthesized mammography detected 3.5 times more invasive cancers than digital mammography alone in the first screening round.2 Moreover, by administering a similar radiation dose during DBT as in 2D mammography,3 we can simultaneously capture a 3D and a 2D image.
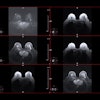
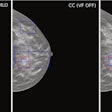
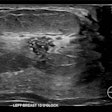
 Clinical images comparing results from the same patient taken on a 2D mammography system (left), using contrast-enhanced software (center), and on a 3D mammography gantry (right). Figure courtesy of Hologic.
Clinical images comparing results from the same patient taken on a 2D mammography system (left), using contrast-enhanced software (center), and on a 3D mammography gantry (right). Figure courtesy of Hologic.
The benefits of DBT are evident and its utilization in breast cancer screening is expanding across Europe. This has meant an increase in the volume of images that radiologists have to review. This workload can be alleviated by using AI integrations. From their initial application in computer-aided detection (CAD) to the current era of deep learning, AI can play a significant role in supporting radiologists in screening images.
Deep learning AI-based solutions assist radiologists in identifying suspicious areas within mammograms, surpassing traditional CAD algorithms in specificity and overall effectiveness.4 As AI continues to evolve, it has the potential to significantly enhance radiologists' expertise and accelerate the review process.
While it augments radiologists' ability to detect additional cancers, AI also optimizes workflow by providing valuable insights prior to study review. It achieves this by providing essential metrics during image acquisition that allow radiologists to sort and prioritize cases based on their complexity. This technology's potential to mitigate interpretation variations has already sparked interest, especially in underserved areas.
In the future, AI is expected to become more personalized and comprehensive, drawing from diverse training data to extend the benefits of the technology to more women. Undoubtedly, the integration of AI is the future of mammography as it offers many opportunities for advancement in breast cancer screening practices.
More options for supplemental screening
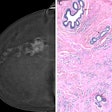
For those patients who require supplemental screenings following an inconclusive mammogram due to dense breast tissue or other risk factors, recent studies have found that contrast-enhanced mammography (CEM) and MRI have comparably high sensitivity in the detection of breast lesions.5 Performed on a facility's existing DBT system, CEM uses the same physical imaging principles as CT and MRI: the contrast agent moves throughout the breast tissue via blood flow and accumulates where lesions are forming and growing.
As more research continues to show that the performance of CEM can potentially match that of MRI,6 this technology is expected to see increasing adoption and utilization. This is important as MRI remains out of reach for some women due to accessibility. New investigations have shown extensive wait times for patients stretching from months to even years for MRI appointments. Furthermore, CEM can be used for staging patients who cannot undergo an MRI, such as those with claustrophobia, those who are allergic to gadolinium, and women who are obese.7
Building on the wider adoption of CEM is the recent introduction of contrast-enhanced biopsy. This is capable of potentially targeting and acquiring samples in lesions identified with CEM. By adding these advanced tools to an existing DBT gantry, facilities can manage patient scheduling and imaging in-house, thereby reducing the opportunity for delays.
When navigating evolving breast screening recommendations and the dynamic landscape in Europe, clarity is paramount for both patients and healthcare providers. Understanding the updates to the EC recommendations and exploring current tools like DBT could potentially have benefits for patients. Additionally, advances in supplemental screening technologies like CEM and emerging AI software offer promising momentum in our field. Maximizing these tools' benefits requires widespread awareness to ensure they are used throughout Europe.
Dr. Eva Pallwein is a specialist in radiology at the Radiology Institute, Steyr Health Centre, Steyr, Austria.
The comments and observations expressed herein do not necessarily reflect the opinions of AuntMinnieEurope.com, nor should they be construed as an endorsement or admonishment of any particular vendor, analyst, industry consultant, or consulting group.
References
- Friedewald SM, et al. "Breast cancer screening using tomosynthesis in combination with digital mammography." JAMA 311.24 (2014): 2499-2507.
- Weigel S, Heindel W, Hence H-W, et al.: Breast Density and Breast Cancer Screening with Digital Breast Tomosynthesis: A TOSYMA Trial Subanalysis; Radiology, 2023;306(2):e221006
- Svahn TM, Houssami N, Sechopoulos I, et al. Review of radiation dose estimates in digital breast tomosynthesis relative to those in two-view full-field digital mammography. Breast, 2015 Apr;24(2):93-9.
- Kshirsagar A. Comparison between ImageChecker CAD and GAID algorithm on sequestered FDA database. 2023. Refer to Hologic document (DHM-14593)
- Gelardi F, Ragaini EM, Sollini M, et al. Contrast-Enhanced Mammography versus Breast Magnetic Resonance Imaging: A Systematic Review and Meta-Analysis. Diagnostics (Basel). 2022 Aug 4;12(8):1890.
- Lobbes M, Heuts E, Moossdorff M et al. Contrast enhanced mammography (CEM) versus magnetic resonance imaging (MRI) for staging of breast cancer: The pro CEM perspective. Eur J Radiol, 2021;142:109883.
- Coffey K, Jochelson MS. Contrast-enhanced mammography in breast cancer screening. Eur J Radiol, 2022 Nov;156:110513.