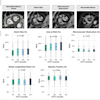
A patient had to make an agonizing decision to terminate her first pregnancy at 25 weeks after a midwife said she was too busy to read two ultrasound exams showing serious fetal abnormalities, according to a report issued on 21 June by the New Zealand authorities. The problems with the pregnancy could have been picked up a month earlier, the report found.
 Rose Wall was head of the investigation. Photo courtesy of the Health and Disability Commissioner.
Rose Wall was head of the investigation. Photo courtesy of the Health and Disability Commissioner.In her analysis, Rose Wall, the Deputy Health and Disability Commissioner, criticized the midwife -- known simply as RM B and referred to as a self-employed registered midwife in her first year of practice -- for failing to read the results of two ultrasound scans. Wall noted that it was a basic requirement of any health professional to refer to scan results, and RM B had breached the patients' rights code.
The patient (Mrs. A) made repeated requests for information from the midwife about these exams, but she was met with unfulfilled promises or silence from the midwife, Wall wrote.
"I should have been referred to a specialist four weeks ago after my 16-week scan ... I had specifically asked you twice about the radiology report and didn't get a reply," Mrs. A wrote to RM B in a text message.
Key findings
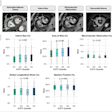
The investigation found that Mrs. A's 12-week ultrasound scan showed her baby was measuring nine days smaller than her estimated due date, and a scan was organized for the following week. Her next scan at 13 weeks and two days pregnant showed the fetus's chest was small and the baby was still measuring nine days behind the estimated due date, so a 16-week scan was recommended.
The scan results were forwarded to the midwife for review, but she never looked at them. The midwife told the commissioner she was struggling to meet the demands of a lead maternity carer and took on too much work too quickly. At the time, RM B had six clients due to give birth in one month. This equated to 72 clients per year, while the number recommended by the Midwifery Council was between 40 and 50.
Mrs. A's 16-week scan showed the baby measuring 15 days smaller than the estimated due date, and a specialist opinion was recommended. The results of this scan were also forwarded to the midwife, but she told Wall she did not recall whether she read the report and no further action was taken.
The 20-week scan showed the baby was very small, and a specialist appointment was recommended, along with a 32-week scan. Further tests indicated a "syndromic diagnosis with uncertain prognosis" was likely, and Mrs. A decided to terminate her pregnancy at 25 weeks.
Lessons to learn
Wall stated that the case highlights the importance of communication between a woman and her midwife, and the need for junior midwives to recognize their limitations and ensure their caseload is appropriate for their level of experience.
Wall pointed out that RM B had since reflected on these events and decided to stop working as a midwife. She has also made a written apology to the patient.
If RM B ever decides to recommence her work, she should receive all scan and laboratory reports electronically, set up a shared system of electronic notes for midwives in the practice/clinic, and introduce a system of 'tasks to do,' " added Wall.
During the investigation, an independent midwifery expert told Wall that a midwife is expected to read and acknowledge every result.
Wall said the midwife's failure to read the scan results had significant consequences for the advice she was able to give Mrs. A, leading to a missed opportunity for her to be seen by a specialist.
The midwife had minimal support from her peers, Wall wrote. "It was inappropriate and unsafe for RM B to have such a high caseload. In my view, this reflects RM B's lack of awareness of her limitations."
Wall, a nurse by training, was appointed to her current role in August 2013 and has been involved in the public health system for around 30 years. In her bio on the HDC website, she says her priority l is to help people, particularly the more vulnerable who are less able to speak up for themselves.
In February 2016, Wall survived a serious road traffic accident in which her partner, 64-year-old Aucklander Graham Charles Hare, was killed.
Risks of pregnancy
For obstetrics, there needs to be consideration of shared care and a documented structured process for moving care to those with greater skills if something is not right and patients need to understand the importance of this, a source told AuntMinnieEurope.com.
"Too often the risks of pregnancy are downplayed or not understood as it is a natural process. We no longer have firsthand experience of women dying in childbirth so are not aware of this risk. Pregnancy is still one of the most dangerous things young women expose themselves to, especially in developing nations where good health care is lacking or hard to get," the source said.
Her main advice to health care practitioners is not to refer for a test that will not make a difference to management (potentially), have a system to record all referrals for radiology and pathology, and record the receipt of the results and the actions taken. Also, do not send patients for tests if you do not know what to do with the results, she said.
"If the report has something that does not make sense or that is really unusual, get in touch with the reporting specialist and ask for advice: Radiologists are only too willing to help and provide advice" the source added. "If nonmedical practitioners want to engage in activities that are a part of role extension, then they need to understand the responsibility that comes with that role extension (a common example is that pharmacists giving flu vaccinations need to be skilled at treating anaphylaxis)."