CT lung cancer screening can be optimized by recognizing the significant differences in the frequency of noncalcified nodules and also the difference in the frequency and aggressiveness of diagnosed cancers from baseline to annual repeat screening rounds, according to lung cancer expert Dr. Claudia Henschke, PhD.
Henschke and her team reviewed more than 65,000 baseline CT lung screenings to identify the frequency and percentages of the largest noncalcified nodules, lung cancer cell types, and survival rates. They found high percentages of each in baseline rounds, which in turn provides information on length and lead-time biases.
"The results of the baseline and annual repeat rounds of screening form the basis for the different recommendations for the threshold and workup of noncalcified nodules identified in baseline and annual repeat rounds of screening in the I-ELCAP [International Early Lung Cancer Action Program] protocol," wrote Henschke, from the radiology department at Icahn School of Medicine at Mount Sinai in New York (European Radiology, 5 October 2017). "Critical for an optimal regimen of screening is that it is continually updated as new diagnostic and therapeutic approaches are introduced."
The base is the basis
The earlier the cancer is detected, the more likely it can be cured. However, not all cancers are aggressive or fast moving. How is a physician supposed to differentiate between a nodule that needs treatment right away and those that may be treated more conservatively?
The answer: baseline screening. Using baseline screening, radiologists can determine if nodules are new and how much they've grown, as well as identify the lung cancer cell type.
"These differences are inherent consequences of screening for any cancer, typically referred to as length and lead time biases," the authors wrote.
To determine the differences between baseline and annual screenings, the researchers used the I-ELCAP screening database to determine the frequency and percentages of nodules by nodule consistency, cell types of diagnosed lung cancers, of different cell types, and long-term survival rates, separately for the baseline and subsequent annual rounds.
The 65,374 screens come from institutions that participated in I-ELCAP between its start in 1992 and 31 December 2014, conducting CT lung screens of current, former, or never smokers age 40 and older with no prior diagnosis of lung cancer. Participants categorized as high risk included all former and current smokers age 55 and older who had a history of 30 pack years or more of smoking. Participants categorized as lower risk included all never smokers and smokers who had a history of fewer than 30 pack years of smoking who did not meet the high-risk criteria.
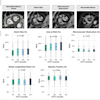
Among the baseline screenings, 28,279 (43.3%) cases had at least one noncalcified nodule.
| Frequency of noncalcified nodules (NCNs) and diagnosed lung cancer | ||||||
| Size of largest NCN (mm) | ||||||
| < 6 | 6-9 | 10-14 | 15-30 | 31+ | Total | |
| Baseline round cases with NCN | 21,681 | 4,399 | 1,291 | 781 | 127 | 28,279 |
| Baseline round cases of diagnosed cancer | 73 | 148 | 186 | 264 | 66 | 737 |
| Annual repeat rounds cases with NCNs | 3,281 | 972 | 438 | 231 | 37 | 4,959 |
| Annual round diagnosed cases of cancer | 46 | 54 | 44 | 25 | 10 | 179 |
The number of diagnosed cases of lung cancer manifesting as a solid noncalcified nodule was higher than those manifesting as subsolid (540 versus 197), but the percentage of diagnosed cases among all manifesting as a solid noncalcified nodule was half that for subsolid ones (2.3% versus 4.5%), the researchers found. For cases in which the largest noncalcified nodule was less than 15 mm, the percentage of those diagnosed with lung cancer was similar among the solid and subsolid noncalcified nodules. For cases in which the noncalcified nodules were 15 mm or larger, the percentage diagnosed with lung cancer increased for larger solid noncalcified nodules but not for larger subsolid ones.
Of the 157 diagnosed cases manifesting as a solid noncalcified nodule, 122 (77.7%) had clinical stage I lung cancer as did all of the 22 cases manifesting as a subsolid nodule, they added. Synchronous primaries were found in 11 (6.1%) of the 179 cases of lung cancer, in nine of the 157 manifesting as a solid noncalcified nodule, and two of the 22 as a subsolid nodule. Median size was 8.8 mm -- significantly different from the size in the baseline round.
Looking specifically at lead time, it was lowest for the most aggressive cancer, small cell carcinoma (1.3 years), followed by squamous cell (2.4 years), adenocarcinoma manifesting as a solid nodule (5.8 years), adenocarcinoma manifesting as a subsolid nodule (10.2 years), and typical carcinoids (18.2 years). The remaining other cell types had a combined lead time of 3.1 years. Overall, considering all cell types, the lead time was 4.7 years, according to the researchers.
The 10-year Kaplan-Meier lung cancer-specific rate for all patients with diagnosed lung cancer was 84% and 88% for the baseline and annual repeat, respectively. The slightly higher rate for annual repeat patients compared with baseline patients was not statistically significant. The combined rate was 85% and median follow-up time for all cases was 79 months.
The Kaplan-Meier lung cancer-specific rate for the high- and lower-risk group was 81.9% versus 88.5% for the baseline and 86.3% versus 91.0% for the annual repeat rounds, which again were not significantly different.
What it all means
"The aggressiveness of lung cancers diagnosed in the baseline round is different from those diagnosed in annual repeat rounds," the authors wrote. "This was demonstrated by the higher frequency of cases of adenocarcinomas, which have higher Kaplan-Meier survival rates identified in the baseline round. It was also demonstrated by the rank ordering of cancer cell types by their lead times."
As information about the appearance and growth rates of small, early lung cancer increased, the definition of a nodule that is positive for cancer in the baseline round has changed from no size threshold in the initial ELCAP protocol to 5 mm by 2000, and finally to 6 mm in 2016. The threshold of 3 mm for a positive result of annual repeat screening, however, has not changed since 2000.
"The results do not fully reflect what could be achieved by CT screening in the future, but show that overall annual CT screening has provided a lead time of 4.7 years, which provides a lower limit of what could potentially be achieved," the authors wrote. "Clearly, the earlier the cancer is detected, the more likely it can be cured, and this together with further improvements in CT technology or other technologies should make screening even better."