Radiologists need to streamline the care they provide to save money and maximize the value of their images -- or else others will do it for them, according to a keynote lecture at the recent 2013 Society for Cardiovascular Magnetic Resonance (SCMR) meeting.
In his closing address, Dr. Frank Rademakers, PhD, from University Hospital and KU Leuven in Belgium said radiologists are drawn to focus on the beauty and integrity of their images in the service of a correct diagnosis. But beauty is in the eye of the beholder, and from a clinical point of view, beauty is found in patient-centered care, said Rademakers, who is medical director and head of cardiovascular imaging and dynamics at KU Leuven.
 Patients want us to be nice to them, according to Dr. Frank Rademakers, PhD.
Patients want us to be nice to them, according to Dr. Frank Rademakers, PhD.
"What patients are really wanting to get from us as caregivers is survival, outcome, quality, and attitude," he told delegates on the final day of the SCMR's 16th annual meeting in San Francisco on 3 February. "They want us to be nice to them."
Furthermore, the economic crisis "means that healthcare has to keep track of what it costs, and we will be looking at added value, quality over cost, more than anything else," he added. Today's healthcare dollars are spent mainly on diagnosis and treatment when the lion's share needs to be spent on prevention, which yields far greater returns and correctly refocuses attention on the patient.
In a positive trend, the past few years have actually seen a decline in cardiovascular mortality -- data from the Heart Lung and Blood Institute of the National Institutes of Health (NIH) in the U.S. show hospital discharges for cardiovascular disease have fallen a little, "but we all know we will be challenged with even greater costs because of the aging of the population and the increased prevalence and incidence of cardiovascular disease with age," Rademakers said. Fortunately, oncological problems tend to decrease in this same aging population.
NIH data also confirm cardiovascular care is by far the most expensive component of patient care and will remain so for some time, Rademakers said.
Doing more with less
"We've had a boom in cardiology in the developments, both pharmaceutical and technical over the years, but it seems we've reached the limit," he said. FDA and equipment manufacturers' data show declines in the numbers of new drugs coming to market, and declines in both new drugs and technical developments entering the development pipeline -- and imaging is leading this decrease, Rademakers said.
"At the same time we will be dealing with a decreased inflow of cardiologists into the field, which means there will be less of us dealing with more patients," he said.
The latest data also confirm that in the Western world, risk factors both behavioral and inherited are powerful predictors of cardiovascular disease and outcomes, which hinge to a great extent on diet and exercise.
Yet no treatment can approach the power of prevention, which is also by far the cheapest approach, "which means that prevention and preventive measures are what the regulators and stakeholders are asking for, and you know as well as I do that today in cardiology and medicine in general, most of the costs go toward the last months of a person's life, not in prevention, and we will absolutely need to change that," Rademakers said.
"We will need to shift from treating disease to promoting health, and if we want to do that, MR is really at the front line," he stated.
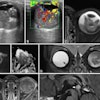
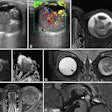
Why? Because MRI sees the very earliest signs of early atherosclerotic disease, for example, making it ideal for a new focus on prevention to steer the patient toward the avoidance of more damage later on, he said.
Fryback et al described the hierarchy of diagnostic efficacy, which begins with the technical quality of the exam, followed by sensitivity and specificity measures, and today more and more the exam's prognostic ability, at task at which cardiac MR excels, he said.
"But we need to move beyond that and say that we affect and improve patient management and do so at the most efficacious level and also at the lowest possible level with respect to societal costs," Rademakers said.
As Schoenhagen et al noted in an editorial last year, it is only by looking at imaging's relative survival benefits that clinicians will be able to show these techniques are a necessary component for improving patient outcomes, he said. Survival data have not played much of a role in imaging in the past, but will need to be a big part of the future, he said.
MR's role in a leaner medical future
"We need to move from just thinking about coronary-focused lesions to a set of problems where it is obviously just one of the issues, but also material dysfunction, microvessel dysfunction, vasospasm, inflammation, and blood pool are equally important and need to be addressed as well," Rademakers said.
To begin, there's a well known lack of association between degree of stenosis and coronary flow reserve (CFR) -- so invasive fractional flow reserve (FFR) is now the leading way of determining which lesions need treating, while a variety of techniques can be used to look at coronary flow reserve. But there's little real interaction between FFR and CFR, and research is revealing why, according to Rademakers.
For example, Gold et al showed resting flow only decreases for very severe stenosis, while maximum flow drops rapidly for >50% stenosis, Rademakers said. The FAME trial put this concept into practice, demonstrating that FFR-guided percutaneous coronary intervention (PCI) yielded better outcomes than angiography-guided PCI. However, the COURAGE trial showed medical therapy and PCI yielded similar patient outcomes. Meanwhile, FAME 2 found FFR-guided PCI was driven only by revascularization, and compared to medical therapy did not reduce deaths or myocardial infarctions. However, the FAME 2 trial was stopped prematurely and therefore is more difficult to interpret.
"So what PCI really does, it seems for the moment, is to prevent early revascularization driven by clinical symptoms, but it has no effect on mortality or myocardial infarction," he said.
Closely related is ischemia, which also merits more research, he said. Many patients with coronary disease have normal FFR but reduced CFR -- or vice versa. Many patients have abnormal FFR but normal coronary flow reserve, and the latter group may not benefit from revascularization.
For evidence, the MASS trial concluded revascularization either with PCI or CABG is more expensive and less effective than initial optimal medical therapy, he said.
"I would say from this that patients do not die from coronary stenosis, they die from arrythmias related to ischemia and scar, and it is the ischemia we need to treat, not the coronary lesions," Rademakers said.
Rademaker said his group's model showed an association between perfusion and function, and a perfusion decrease in the setting of no coronary stenosis. So looking at the cardiac function-perfusion relationship could be another way to identify functional abnormalities due to cardiac ischemia, although BOLD sequences and spectroscopy can also do the job, he said.
"Added value these days is the buzzword in health economics and we need to look at that with a focus on prevention," he said. "I think we need absolute quantification of flow to be able to identify decreased flow reserve."
Comprehensive functional information, including low metabolism, and perfusion, is needed to identify true ischemia, Rademakers said.
"CMR can provide most if not all of the information that is required here, and I think it has a bright future as long as we keep an eye on adding that value," he concluded. "We need to control our costs, or someone will do it for us."