For a lung cancer screening program to to be successful, patients must be carefully chosen, the program must form part of a wider prevention plan, and strict diagnostic criteria and high standards of technological and medical intervention are essential, according to Dr. Hans-Ulrich Kauczor, professor of radiology at Heidelberg University Hospital in Germany.
Germany's healthcare system has early detection programs for breast, cervical, colon, and other cancers. In recent years, bronchial carcinoma has been added to the list of cancers for which screening can be effective, using a low-dose CT scan of the lungs. Some features of latest-generation CT scanners, such as iterative reconstruction, require only about a fifth of the radiation dose normally required for diagnostic CT scans of the lungs, thus reducing the risks associated with radiation exposure.
CT screening can reduce lung cancer mortality by 20%
The large, randomized U.S. National Lung Screening Trial (NLST) shows that low-dose CT can be effective. "The study found that screening achieved a one-fifth reduction in mortality from bronchial carcinoma in people who smoked at least one pack of cigarettes a day for at least 30 years," noted Kauczor, who is a keynote speaker at the 99th German Radiology Congress (Deutscher Röntgenkongress, RöKo 2018). "Overall mortality was also lower."
 Dr. Hans-Ulrich Kauczor.
Dr. Hans-Ulrich Kauczor.The U.S. has now established an official screening program based on the NLST in which a CT scan is offered to long-term smokers ages 55 to 80. Kauczor, who will be giving an overview of the subject at the congress, chairs a newly established committee on lung cancer screening at the German Radiological Society. This committee works closely with other professional bodies, the federal radiation protection department, the Gemeinsamer Bundesausschuss (the committee that decides which treatments are eligible for funding), health insurance funds, and political parties. It is aiming to introduce a screening program into the German healthcare system.
This is made easier by a new German radiological protection act, based on European Union (EU) legislation, which will allow healthy people to undergo x-rays under certain circumstances. So far, only the early breast cancer diagnosis program has been granted a one-off exemption from the rules.
Using a comprehensive risk model to identify patients
As with all early diagnosis programs, early lung cancer screening must strike the right balance between identifying as many people as possible who have the disease and minimizing the number of individuals who are wrongly diagnosed. "Patients with false positives may undergo unnecessary intervention, and we must avoid that as much as we can," said Kauczor in a precongress interview.
Germany should operate a different screening program to that of the U.S., focusing on a relatively narrow target group, he noted. "It will work only if we manage to reach people who are at high or very high risk," he said. A comprehensive risk model should include smoking 20 cigarettes a day as one criterion, but it should also incorporate other factors that assess individual risk more effectively, such as age, gender, family or personal history of cancer, and contact with other potential carcinogens that can make lung cancer more likely.
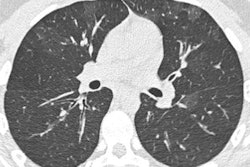
 A 59-year-old heavy smoker participated in the German lung tumor screening and intervention (LUSI) study. A: Baseline examination without round lesion. B: One-year follow-up: new 15-mm round lesion (arrow). The histology showed a poorly differentiated pT1b adenocarcinoma. Five years later, the patient was still tumor-free. All images courtesy of Dr. Hans-Ulrich Kauczor.
A 59-year-old heavy smoker participated in the German lung tumor screening and intervention (LUSI) study. A: Baseline examination without round lesion. B: One-year follow-up: new 15-mm round lesion (arrow). The histology showed a poorly differentiated pT1b adenocarcinoma. Five years later, the patient was still tumor-free. All images courtesy of Dr. Hans-Ulrich Kauczor.Comprehensive prevention program
A screening program must also meet high technical and medical standards. For example, it must lay down clearly defined participation criteria, diagnostic limits, and quality control mechanisms so the next and more invasive diagnostic steps are taken only if the patient is truly at high risk.
CT screening should look for the typical round lesions of lung cancer and also early-stage COPD or atherosclerosis, both of which are caused by smoking, according to Kauczor. "And finally, it's vital that CT screening for lung cancer should include stopping smoking and prevention programs if it's to be comprehensive and attractive to smokers," he noted. This is also the message of a joint position paper by European radiology and pulmonology bodies.
RöKo 2018 takes place at the Congress Center in Leipzig from 9 to 12 May.
Editor's note: This is an edited version of a translation of an article published in German online by the German Radiological Society (Deutsche Röntgengesellschaft, DRG). Translation by Syntacta Translation & Interpreting. To read the original version, visit the DRG website.