I became a consultant radiologist in 1986, working at the old Bromley Hospital in South London. Looking back now, working conditions were unbelievably primitive. The only digital imaging was the offsite CT scanner, and all reporting was from hard copy with a secretary sitting to my left typing onto paper reporting proformas. These reports were then stored in cabinets. When we moved images around, we had to physically move the film packets, and the management of film packets was a major task. When a film packet was missing, clinicians always assumed it was the fault of radiology!
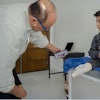
 By the mid-1980s, radiologists were at the center of the reporting process, working remotely from a monitor (Gitlin, 1986).
By the mid-1980s, radiologists were at the center of the reporting process, working remotely from a monitor (Gitlin, 1986).
All that has changed and we now do soft-copy reporting and transfer images electronically within the hospital and between hospitals in the group. We also send images directly to tertiary referral centers. So how did all this teleradiology develop?
The first use of teleradiology was probably in 1959, when Dr. Albert Jutra linked two hospitals in Montreal. The hospitals were 5 miles apart, and Jutra used a coaxial cable to share videotaped fluoroscopic studies. Jutra was very perceptive and suggested a network connecting hospitals to doctors' offices to facilitate the exchange of radiological information, and he emphasized the need "to determine the efficiency, usefulness, and economy of roentgenologic telecommunication."
There were further developments in the 1960s. Following an airplane crash at Logan Airport in Boston in 1962, a new medical department was set up at the terminal by Dr. Kenneth Bird. Using a telemedicine link, he connected Logan with the Massachusetts General Hospital, located 2.7 miles away. This microwave link was then used by R. Murphy and co-workers in 1970 to transmit chest radiographs for remote interpretation. Murphy selected 100 chest radiographs of patients from a tuberculosis hospital. A panel of three doctors reached agreement in 92 of the cases, and when compared with the radiology report, there was 77% agreement.
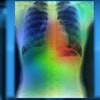
 Digitizing a radiograph using a video camera with freeze frame (Gitlin, 1986).
Digitizing a radiograph using a video camera with freeze frame (Gitlin, 1986).
Further studies were performed in the 1970s using a slow-scan television, and images were sent on ordinary telephone lines; while images were acceptable for low-resolution nuclear medicine, images they were not acceptable for radiographs. By 1976, Lewis Carey in Ontario was using the Hermes satellite to investigate interactive telecommunication within a regional healthcare system. For more than five months, Lewis Carey and his team provided 297 radiological consultations and remarkably gave live supervision to 14 television fluoroscopic examinations that were being performed by a radiologic technician. Carey concluded the consultation service was 90% as effective when compared with direct film viewing.
There were more teleradiology studies in the 1980s in the U.S., with a large field trial in 1982 located at the Malcolm Grow Hospital in Andrews Air Force Base, which served as a central location providing radiographic interpretation to one civilian and three military clinics. The radiographs were scanned using a video camera with a freeze frame constructing a 512 x 512 x 8-bit matrix. The digitized x-ray images from the remote clinic were sent via telephone lines to the central medical center and the radiological report was returned again by telephone lines. The results of the trial were successful and in 1984 the Uniformed Services University in Bethesda, Maryland, replaced Malcolm Grow Hospital as the hub linking the four sites. In the 1984 study, a matrix density of 1024 x 1024 pixels was used. The radiographs were scanned and converted to a digitized image. The results of the 1982 and 1984 trials were very encouraging with only a few discrepancies between the video and film reports.
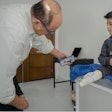
 Communication links between clinics and medical centers (Gitlin, 1986).
Communication links between clinics and medical centers (Gitlin, 1986).
In 1985, Lewis Carey reviewed teleradiology and predicted that, "Improved access to radiologists, 24 hours a day, will provide a level of service heretofore not possible." This has proved to be the case and studies are now routinely reported by radiologists at home or transmitted between hospital sites for reporting. Images may also be reported in another country but there are clinical and legal concerns. There is a danger that teleradiology will adversely alter the relationship between the radiologist and clinicians, and such a service needs to be used with caution.
In 1986, I could almost forget when I was on-call because I was called in so infrequently. We now offer a 24/7 service, with overnight scans being reported via a teleradiology link. However, technology continues to advance apace and as an example it is now possible for radiological images to be reviewed on a tablet computer.
References
- Carey LS. Teleradiology: Part of a comprehensive telehealth system. Radiol Clin North Am. 1985;23(2):357-362.
- Gitlin JN. Teleradiology. Radiol Clin North Am. 1986;24(1):55-68.
Dr. Adrian Thomas is chairman of the International Society for the History of Radiology and honorary librarian at the British Institute of Radiology.
The comments and observations expressed herein do not necessarily reflect the opinions of AuntMinnieEurope.com, nor should they be construed as an endorsement or admonishment of any particular vendor, analyst, industry consultant, or consulting group.