Caution persists when it comes to applying lung cancer screening, as the wait goes on for more conclusive mortality data, but consensus is growing that lung cancer screening is likely to become more cost-effective, according to a leading U.K. expert.
In the run up to the British Institute of Radiology (BIR) annual congress in November, the BIR interviewed Dr. Nicholas Screaton, a consultant radiologist at Papworth Hospital National Health Service (NHS) Foundation Trust in Cambridge and senior editor of the British Journal of Radiology. BIR Content Development Editor Miranda Wilson-Wood spoke with Screaton in a podcast posted on 16 October.
"I think all would agree more work needs to be done to identify what is the most cost-effective and most effective way of performing lung cancer screening," he said. Part of that could be more refined participant selection.
Split down the Atlantic
Lung cancer is one of the most common cancers and most fatal -- likely because two-thirds of patients with lung cancer present at a time when they are not suitable for curative treatment, according to Screaton. These patients present with typically nonspecific symptoms such as breathlessness or weight loss. The patient's general practitioner (GP) will request an x-ray, which is relatively insensitive in picking up early disease. If the chest x-ray comes back abnormal, the patient will receive a CT scan, which is far more sensitive than x-ray.
 Dr. Nicholas Screaton.
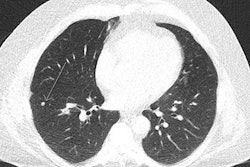
Dr. Nicholas Screaton.Because of this chasm between x-ray and CT, and CT's superiority in detecting lung nodules, clinicians started to question whether CT could be used to screen for lung cancer back in the late 1990s and early 2000s. Early observational studies showed low-dose CT (LDCT) effectively identified lung nodules, but without a randomized controlled trial, it was impossible to confirm definitively if LDCT improved lung cancer specific mortality. That all changed in 2011 with the National Lung Screening Trial (NLST).
The NLST was stopped early in 2011 because it showed a significant impact on outcomes using lung cancer screening -- a 20% reduction in lung-cancer related mortality in the screened group compared with the control group. The results were enough to convince the medical community in the U.S. to start using LDCT to screen for lung cancer; so much so that the U.S. Preventive Services Task Force (USPSTF) issued a draft recommendation offering annual CT screening to individuals who met the NLST criteria -- namely, individuals between the ages of 55 and 80 who had smoked for at least 30 pack years and who had smoked regularly during the past 15 years.
However, Europeans haven't been so quick to board the lung cancer screening bandwagon. Several countries performed their own lung cancer trials, including the U.K. and Italy but most policymakers seem to be waiting for the results of the Dutch-Belgium NELSON trial.
"The NELSON trial is pending reporting on its mortality figures, and I think is one really important piece of the jigsaw that is still missing," Screaton said.
While some countries are holding off until receiving NELSON data, in the U.K., several major centers, including Manchester, Leeds, and North London, have launched or are in the process of setting up lung cancer screening services.
"I think as the centers are setting up their services it may add extra pressure that may see us performing broader, NHS-funded lung cancer screening," he said.
Making screening better
Regardless of whether a center has adopted lung cancer screening, more could be done to improve the process, according to Screaton. The NLST identified high-risk individuals purely on age and smoking history, but clinicians could also perform personalized risk prediction to identify high-risk individuals. They could look at other variables such as a history of previous cancer, a family history of cancer, and a previous history of pneumonia. In turn, the risk-prediction models could purify the lung cancer screening pool, so to speak, and make the whole process more cost-effective by screening fewer people to identify more lung cancers.
Another way to improve screening is with the use of nodule volume, which is proving to be a more precise measurement of change in tumor size.
"As time has gone by, nodule management protocols have generally increased the size of a nodule that is considered actionable, and, as I've mentioned, nodule volumetry is, I think, going to play an increasingly important role because it is able to assess the rate of growth of a nodule, its volume doubling time," he said. "And the volume doubling time of a lesion correlates with how aggressively it's behaving and, therefore, potentially a slow-growing lesion can be managed conservatively, not resected."
And if lung cancer screening becomes the norm? As radiologists are already constrained, using computer-aided diagnosis (CAD) could be a good support, Screaton added.
To listen to the full podcast, visit the BIR website.