As patient numbers continue to rise, diagnosis and follow-up will rely increasingly on multiparametric imaging, and structured reporting and advanced technology will be key to optimizing patient management. This means that radiologists will have to become more familiar with these areas, according to Dr. Maximilian Reiser, professor of radiology and director of clinical radiology at Ludwig Maximilian University in Munich.
 Dr. Maximilian Reiser. Image courtesy of the German Radiological Society.
Dr. Maximilian Reiser. Image courtesy of the German Radiological Society.Precision medicine is imaging's biggest challenge, noted Reiser in a precongress interview with AuntMinnieEurope.com. On the opening day of the national German radiology congress (DeutscherRöntgenkongress, RöKo 2016), which takes place in Leipzig from 4 to 7 May, he presented the latest thinking on how imaging will shape the future of patient care across Europe. His talk was part of a session that also included perspectives from the U.S. and Asia.
Reiser believes that obtaining precise information to characterize disease processes in patients that will allow for tailor-made therapies will be achieved predominantly in three ways:
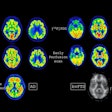
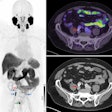
Multiparametric and quantitative imaging. Multiparametric and quantitative imaging will soon be incorporated into daily practice. Such imaging, which combines morphological information with functional, metabolic, and molecular insights, can yield a more precise assessment of diseases. Perfusion and diffusion MRI, spectral CT, and hybrid systems, such as PET/CT, are increasingly used for this purpose.
"With advanced IT technologies these imaging data can be employed for radiomics, which bring higher precision in diagnosis, assessment of prognosis -- for example, disease-free survival in tumor patients -- and selection of appropriate therapy, such as the most effective drugs in cancer therapy. With diffusion-weighted imaging [DWI] the aggressiveness of prostate cancer can be predicted, facilitating the choice of whether to perform aggressive treatment or to wait and see," Reiser said. "Imaging results should be measured quantitatively. It's not enough to say, for example 'strong diffusion restriction.' Whenever possible we should put a number on it."
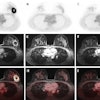
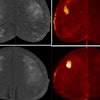
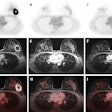
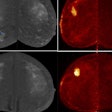
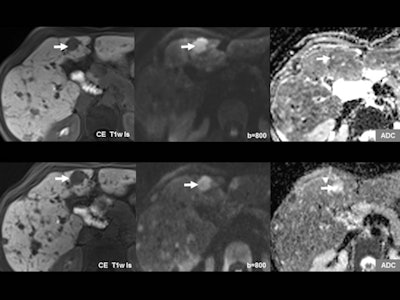 Diffusion-weighted imaging (DWI) can give information beyond that provided by morphological scans. In this case, liver metastasis of a neuroendocrine tumor is shown before (upper row) and after (lower row) therapy. While no change is seen on the contrast-enhanced scans (left), DWI and apparent diffusion coefficient (ADC) (middle and right) show an increase in diffusion that indicates response to therapy. Images courtesy of Dr. Christine Schmid-Tannwald, Ludwig Maximilian University, Munich.
Diffusion-weighted imaging (DWI) can give information beyond that provided by morphological scans. In this case, liver metastasis of a neuroendocrine tumor is shown before (upper row) and after (lower row) therapy. While no change is seen on the contrast-enhanced scans (left), DWI and apparent diffusion coefficient (ADC) (middle and right) show an increase in diffusion that indicates response to therapy. Images courtesy of Dr. Christine Schmid-Tannwald, Ludwig Maximilian University, Munich.Structured reporting. The second way that precision medicine would be supported is through structured reporting, which can help clinicians harvest the specific information obtained by imaging.
"Reports shouldn't comprise free text which changes from radiologist to radiologist and can be interpreted differently depending on the clinician. Radiologists need to know the blueprint for informative text, and provide the data that oncologists want to know, such as growth, regression, or new sites of manifestation," he commented.
Deep machine learning. Multiparametric/quantitative imaging and structured reporting go hand in hand with deep machine learning. This third tool will become increasingly present in the diagnostic process, helping to establish personalized medicine as the norm. Such advanced technology will also allow radiomics to gain ground, particularly in oncology prognostics.
"The prospect of using [deep machine learning] in routine practice is both frightening and exciting. There is no immediate job danger from machine learning, as there are plenty of additional duties, such as making quantitative imaging valuable to clinicians, that can only be carried out by radiologists. Moreover, machine learning and IT support in making radiological diagnoses may help departments cope with the ever-increasing number of exams and workforce shortfall," he said.
Radiology will benefit from a growing number of radiology equipment vendors and IT companies from China and other Asian countries, as well as from Europe and the U.S. This will result in converging practice across the world, according to Reiser, who is editor in chief of the journal European Radiology. Furthermore, the scientific radiological community is also becoming increasingly significant.
"Within the past two and a half years, I have witnessed a rising number of submissions to European Radiology from non-European countries such as South Korea, Singapore, Taiwan, Japan, and India. This tells me that radiology really is a global community," he remarked. "The globalization of radiology is a good thing, but this puts pressure on the specialty to become more effective, namely as a conduit for precision medicine."
Economic factors
Even with the trend for precision medicine and the support of efficient and integrated IT systems, hospitals will be faced with the challenge of there being more patients to treat but only a fixed amount of money available: imaging departments will inevitably have more work to do.
Health systems everywhere will be more prone to "economical thinking" and will push for imaging and IT services to improve and extend output while remaining cost-effective, Reiser continued. Budget restraints and higher patient throughput mean that healthcare providers will need to maintain cutting edge -- yet cost-effective -- imaging services.
He warned that the shift toward more complex imaging studies and analysis such as volumetric CT assessment and radiomics in order to obtain higher levels of precision necessitated improved processes, high-performance workstations, and better organized departments. Decisions by healthcare providers and insurance companies, however, would lead to major differences between regions.
 Radiomics will become increasingly useful in diagnostics and prognostics, particularly tumor-free survival for oncology patients, and therapy selection, but this will be largely dependent on the development of deep machine learning. Figure courtesy of Drs. M. Ingrisch and B. Ertl- Wagner, Ludwig Maximilian University, Munich.
Radiomics will become increasingly useful in diagnostics and prognostics, particularly tumor-free survival for oncology patients, and therapy selection, but this will be largely dependent on the development of deep machine learning. Figure courtesy of Drs. M. Ingrisch and B. Ertl- Wagner, Ludwig Maximilian University, Munich."Demographics dictate that there is ever more need for medical services, with higher output for proportionally the same -- or lower -- costs. Some departments will not get the 'best' machines, but those which are most economical," Reiser noted. "Hospital departments will need to cope with the 'economical thinking' of other parties."
He reported that since 2007 his department has experienced an increase in exams and interventions by 6.5% each year, but the departmental budget has just been cut by 3%. He also pointed to an increasing proportion of CT, MRI, mammograms, and interventions, compared with x-ray, but these are performed with the same numbers of staff, and added the issue of higher output versus lower budgets was not a problem restricted to radiology. All medical disciplines need to become more effective, but with imaging so key to patient management, efficacy needs to start here, he added.
Although advances in technology and IT are a global trend, differing speeds of development in member states increasingly will lead to varied regional radiology practice in the mid to long term, compounded by national differences in healthcare strategy and budgets. However, legislation in the European Union (EU), championed by the European Society of Radiology (ESR), will continue to yield convergence on imaging policies.
Past president of both ESR and ECR, Reiser described how successful lobbying by the ESR had resulted in the withdrawal of plans for legislation that would have affected the way MRI could be used in patient care. The legislation was in line with the 2004 EU Directive aimed to protect staff from electromagnetic waves and would have indirectly impacted radiographers and radiologists at work.
"Although this initiative had the safety of personnel in mind, maximum exposure levels would have been too low, preventing staff from moving around in the scanner room," he said. "This would have made thorough MRI investigations of some patients, such as children, impossible, and would have had a major impact on practice."